Mental Health History1975Better Services for the Mentally Ill |

|
"We believe that the philosophy of integration rather than isolation which, has been the underlying theme of development still holds good" (Better Services 1975 par 2.17).
Better Services for the Mentally Ill, a 91 page 'White Paper' was presented "by Barbara Castle, as Secretary of State at the DHSS, in October 1975. It was nick-named "Castles in the Air" by one radical group (COPE) because this long-term strategic document, pointing out the general direction the Government "wanted services to take, was prefaced with the statement that little progress could be made until the economic situation improved (p iv).
The Paper placed its emphasis on the provision of a comprehensive range of local services (described later) rather than the closure of asylums:-
"...our main aim is not the closure or rundown of the mental illness hospitals as such? but rather to replace them with a local and better range of facilities. It will not normally be possible for a mental hospital to be closed until the full range of facilities described" (in the paper) "has been provided throughout its catchment area and has shown itself capable of providing for newly arising patients a comprehensive service independent of the mental hospital. Moreover, even then, it will not be possible to close the hospital until I it is no longer required for the long stay patients admitted to its care before the local services came into operation" (par 11.5).
Given the economic situation the White Paper was exceptionally hazy about time scales. Providing the local services it proposed required (at November 1974 prices) an average annual capital expenditure of £30 million by the NHS and £8 million by councils over a 20 to 30 year period (par 11.8). Councils had actually spent only about £3 million in this field in 1974/1975 and although the NHS figure was about that actually spent in 1972/1973, less bad been spent since the health cuts (Priorities 1976 introduction and pars 8.9 + 8.10).
The White Paper said investment on the scale needed would not be possible "over the next three or four years" (par 11.5) but in 1976, by giving 'deprived sectors' 'priority' over general and acute hospital provision, a rate of development was proposed which "if maintained" would enable the 'Better Services' aims to be achieved over most of the country within 25 years (Priorities 1976 introduction and pars 8.9 + 8.10).
Although perhaps not as clear as it might have been, one could deduce from Better Services that many asylums were to maintain an active life well into the 21st century, and the White Paper said (p 88, par l) that they would contain the majority of patients "for many years to come".
The House of Commons was later told (*) that at the end. of 1975 only 8.1% of mental illness beds were in general hospitals so, presumably, over 90% of in-patients were still in the old asylums. 30% of admissions, however, were in District General Hospital units, so mental hospitals clearly contained a disproportionate percentage of long stay patients.
* HC Hansard 19/7/1977 col 404. Cited Mind Information Bulletin August/
September 1977.
During the (now long) transitional period to local services the health authorities were to continue with a 1971 memorandum recommendation to split asylums into "divisions" each serving the district in which local facilities were being developed to replace it.
"In this way it is hoped that staff will increasingly think...in terms of a district service which, wherever it is provided, whether from a mental hospital "division", a general hospital psychiatric unit, a community hospital, or in...supportive work in the community itself, is all part of the same district service." (PP 88-9, pars 3-5. See also HM(71)97, par 14)
The "Old Long-Stay" Patients
A 1961 forecast of how many hospital places would be needed in the
mid 1970s was based on a belief that the 110,000 long-stay
patients in 1954 would have died or been re-habilitated by about 1970
(Tooth + Brooke, 1961, section on "Rate of Reduction of Long-Stay
Population")
In 1971, 30,000 of them were still in hospital, their numbers were only
slowly declining and as almost half were under 65 years old the veteran
residents of the old asylums were unlikely to fade away for several
years (pars 2.4 + 2.15).
In 1971 patients who had been in hospital for five years or more occupied
50% of the beds (England and Vales) and 30% had been in hospital for more
than 20 years
(WHO 1976, pp 8 + 57;
Lader, M. in
Meacher, M. 1979, p.37)
The White Paper referred to some, or all, of these
patients as old long-stay, as distinct from new long-stay
New long-stay patients are those who:
The exact distinction between new and old is not clear. At least four
definitions - each involving a different
concept - appear to me explicit or implicit in the White Paper and its
associated literature. For old long-stay these are:-
According to the 'White Paper a great deal of effort in the 1950s and 1960s
had been put into rehabilitation work with long-stay patients - but in
practice it had rarely proved possible to discharge to the community and
hospitals had lost interest in rehabilitating chronic patients (par 2.12).
Many old long-stay patients, it said, were not in hospital because they
needed specialist hospital services, but because:-
The humanitarian argument was a superfluous gloss. Economic
considerations were to determine that old long-stay residents remained in
the asylums. The Government's
Priorities
paper in 1976 took pains to explain that the network of district services
outlined in Better Services was only intended to take over from the mental
hospitals the care and treatment of new patients. The scale of
facilities would not enable it
Money was, however, to be spent maintaining the physical structure and
improving the standards of decoration, toilet and other facilities in
mental hospitals because this was "essential" to maintain the "morale of
the staff" and to ease the "burden of nursing an increasingly ageing
in-patient population"
(Better Services
1975 p 90 par 12).
The "New Long-Stay" Patients
It was the "new" long-stay - those who remained in hospital despite
modern treatment methods - that the "new pattern" of comprehensive local
services was intended, eventually, to benefit. Sir Keith Joseph had
spoken optimistically of "the small proportion of patients who will
require relatively longer stay" (EC Hansard 7/12/1971 col 280) but
Better Services pointed, out that:-
If of 100 patients entering a hospital, one remains for 10 years and the
others stay an average of only 5 weeks then the one long-stay patient
will use the same amount of bed-space as all the 99 short-stay patients.
An article in the British Medical Journal (7/3/1972) estimated that if
chronic patients represented only 1% of all acute hospital admissions,
after only 7 years they would have silted up half the beds in District
General Hospital Psychiatric Units. (Cited MIND/13, p 7)
Better Services quoted estimates (*) that about one in three of the
newly arising long-stay patients not suffering from dementia needed 24
hour medical and nursing supervision.
They were, predominantly,
patients diagnosed "chronic schizophrenic" - who were "particularly prone
to be slow, -withdrawn and liable to neglect themselves" (pars 4.52 +
4.53). 'Hospital' had to be 'home' as well for such patients and a
ward in a District General Hospital Psychiatric Unit could not provide a
sufficiently domestic
environment for patients who stayed more than a year (par 4.53).
The other two-thirds, with the exception of small numbers in special
categories, did not need hospital care, but were in hospital because the
long-term sheltered accommodation in the community they needed was
virtually non-existent (par 4.52 + Wing, J.K. 1973, P 30).
The White
Paper's
Guidelines for council
accommodation
repeated
guidelines issued in 1972 (DHSS 35/72 par 42) with the emphasis on long-
term accommodation instead of hostels. But the value of such guidelines
depended on councils taking note of them. As late as November 1979, my
local borough, Hackney, recorded in its social services minutes that the
difficulties of its new 20 bed hostel were due to consultants referring
"long-stay clients".
Hospital Hostels A suggested approach to the needs of long-stay
patients who needed residential accommodation with medical and nursing
supervision was a "Hospital Hostel" - a large house, reasonably close
to the psychiatric unit, in which residents could be cared for in a
domestic atmosphere, but with night nursing supervision. By day they
would go to the day hospital, to council day centres or, perhaps, to
sheltered work (pars 4.52 - 4.54).
The first (experimental) hospital-
hostel was established at the Maudsley Hospital, South London, in 1977
(Wing in Wing + Olsen, 1979, p.10).
The Elderly
Patients over 65 formed. 20-25% of admissions to mental illness hospitals
and units in 1975 (par 4.l0) and, as at Whittingham, their care was
mainly being left to the mental hospitals. Better Services suggested
priority development of local services for the elderly to counter the
emergence of this 'two-tier' system.
Assessment of elderly patients' needs should, wherever possible, take
place at home or in out-patient clinics because
Where
this was not possible in-patient assessment should take place in a local
unit even where a District General Hospital psychiatric unit had not yet
been established - small 'joint assessment' units could be provided in the
geriatric department of the District General Hospital (par 4.11).
In its comments on the 1972
memorandum, MIND had stressed the importance of such units pointing out
that in one area only 10% of those admitted to a local assessment unit
were found to be in need of long term hospital care (MIND/9, p 4).
In the new pattern of services, hospital admission, where necessary,
would usually be to a psychiatric unit. In some districts a psychiatrist
with special responsibility for elderly people had been appointed and this
could facilitate links with geriatric physicians, G.Ps and social services
departments (par 4.10).
Community Hospitals for patients with severe dementia needed to be
developed in parallel with, if not ahead of, the District General Hospital
Psychiatric Unit so that the mental hospitals were not
The community hospitals would, normally contain
geriatric and psycho geriatric units for longer stay patients and the
geriatric unit would care for all patients who were significantly
physically ill including demented patients (par 4.15).
In such hospitals
the "interest of friends and relations and local communities" could be
more easily maintained, and the day to day care of patients could be
entrusted to local GPs (pars 4.13 + 4.15).
Adjoining the psychogeriatric unit there should, be a day hospital for
in-patients and patients living in the community (par 4.l6).
With respect to the care of the majority of the mentally infirm: those
living at home (or sometimes in old people's homes) the 'White Paper had
little to say. The DHSS was "examining the advantages and
disadvantages" of various local authority support schemes, "and may issue
guidance...in due course" (par 4.48).
The Future Pattern of Services.
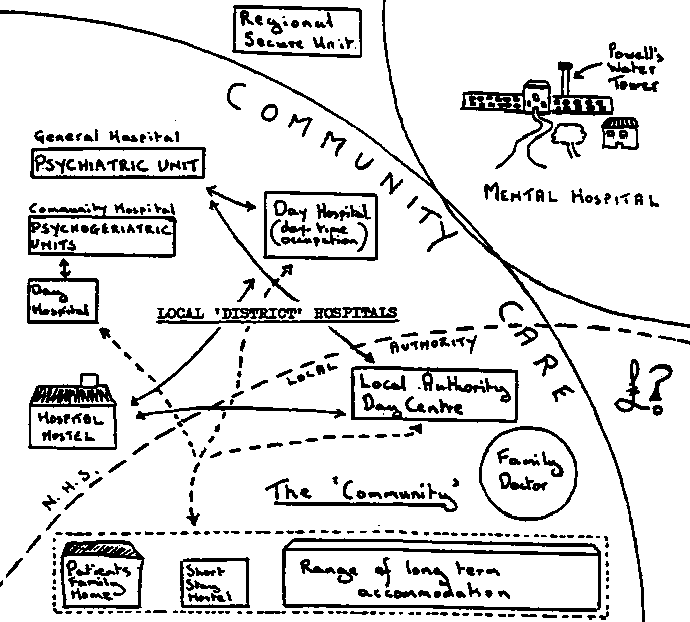
The psychiatric scenario outlined in Better Services is illustrated by
the table (*) and diagram below.
The old asylum, or mental hospital, is outside the community:
It is a self-contained world on its own,
structuring every aspect of its inhabitants' existence day and night, day
after day; and, "because of its location, separating those who reside there
from the lives of families, friends and neighbours - what Goffman called,
in
Asylums, a
Total
Institution.
This is to be replaced by the range
of local facilities shown, although even then the "old long-stay"
residents would remain in the asylum.
In the future pattern of services, hospital facilities be local,
and in-patient treatment avoided.
Where in-patient treatment was unavoidable,
and care continued for any length of time, there would be a distinction
between where the patient resided and where he or she spent the
day.
The
psychiatric unit, for example, was to have "two main functional
components":
a "day activity
area".
The great majority of in-patients would
A range of day-time and evening facilities, including local authority
day centres, sheltered employment schemes and social clubs, would be
required for those living in community accommodation. These would assist
people to maintain an independent life outside hospital and, in some
cases, relieve the strain on families of their living at home. (par 4.28)
In addition to the District level facilities there would be required on a
Regional basis: a 'Regional Secure Unit' (2 beds per 100,000 population)
for patients too disruptive to be accommodated in a District General
Hospital ward, and units
for mentally disturbed children and adolescents (2.25 beds per 100,000
population for each). (Better Services
1975 par 4.63. Norms taken from other
sources).
From Medical to Social Provision
The importance of the strategy outlined in
Better Services
1975 was that it did
not rely on an unrealistic belief in psychiatry's power to "cure" mental
disability. The comprehensive provision it envisaged included long-term
social care for the 'chronic' cases acute psychiatry had been sending to
the mental hospitals.
Hospital staff, the paper noted, saw a hospital's role as an "active
therapeutic one" and were increasingly unwilling to be "social care
custodians" but facilities for social care outside hospital were "not
generally available" (par 2.8). "For 16 years or more" Dr David Owen
told MPs "we have all...paid lip service" to the concept of caring for
most of the mentally ill in the community, but the White Paper showed that,
whilst nearly £300 million (*) was
spent
on hospital services for the mentally ill, in 1973-4 only about £.15
million (*) was spent on Social Services (HC Hansard. 26/1/1976 col 35).
The Government intended to see that, over a period of years, "the balance
of health and social services" was "put right" (par 2.8).
The Government's four main objectives were to expand council services, to
move specialist (hospital) services to local settings, to establish the
right organisational links between sectors and to improve staffing levels
(par 2.22). Alison Wertheimer commented in MIND's magazine that
establishing the right links was the objective that "poses the greatest
difficulties and the greatest hopes" :-
JANUARY 1976: THE BIRMINGHAM SCANDAL.
Between 1970 and 1975 the population of mental illness hospitals was
reduced from 107,977 to 87 .,321 and that of mental handicap hospitals from
55,434 to 49,683 (**).
But how had this been achieved? Some argued it
was by discharging patients to families ill-equipped to cope with them,
to private 'hotels' that exploited them, or onto the streets.
Better Services
1975 acknowledged such things happened, and. said;-
"the public...cannot be expected to tolerate under the name of
community care the discharge of chronic patients without...after-
care...who perhaps spend their days wandering the streets or become
an unbearable burden on the lives of their relatives..• Such
situations do not occur very frequently: but where they do, the
whole concept of community care is placed at risk" (par 2.27)*
[Enter Piorities]
Andrew Roberts likes to hear from users:
© Andrew Roberts 1981-
New and old long stay patients
"despite advances in treatment or staffing" are still becoming chronic
in-patients in "significant numbers" (par 4.52).
"How long before...'new'
long-stay...become 'old' long-stay?" asked COPE (1976, p 26).
"they either need other forms of shelter and support which are at
present not available outside hospital, or have become so accustomed
to hospital life - in some cases so institutionalised - that it would
be inhuman to discharge them from the hospital that has in fact
become their home." (par 4.51)
"to take over responsibility for the
diminishing group of 'old long-stay' patients".
(Priorities
1976 par 8.4)
"While this group may be relatively few...the implications in terms of
resources are quite disproportionate to their numbers"
(Better Services
1975 par 1.16)
* The estimates appear to have been based on Wing, J.K., 1973» but
the 'White Paper also cited research the DHSS had commissioned by Dr
Sheila Mann and Mrs Wendy Cree (Mann, S.A. + Cree, V., 1976).
"the physical uprooting
of an old person is in itself a traumatic experience" (par 4.10).
"left to care for patients who make
heavy demands on nursing staff, often in unsatisfactory physical
conditions" (par 11.19).
* Based on the table in
Better Services
1975 (par 4.64) with the addition of
the figure for "Units for 'New Long-Stay' Patients" from the provisional
estimate in par 4.53.
GUIDELINES FOR SERVICES AT DISTRICT LEVEL
Rates per 100,000 population
Hospital Services
Beds
Day Places
District General Hospital
Psychiatric Unit
50
65
Units for elderly severely mentally infirm patients
30-40
25-40
Units for new long-stay patients under 65
17
Local Authority Services
Beds
Day Places
Hostels
4-6
Long-Stay Accommodation
15-24
Day Centres
60
wards, "or rather residential units", and
"spend the day on a
planned programme in the day hospital...thus having the stimulation of...
a pattern of living which more closely resembles normal everyday life"
(par 4.3)
Better Services
1975 p.ii, par 3. Revenue expenditure (1974 prices)
"The crucial factor in the achievement of the.. .service envisaged.... is
going to be successful joint planning between health and social
services coupled with a shift in resources from the health sector to
... social services." (Mind Out, December 1975 p.12).
 Study
Link
Study
Link
 Andrew Roberts' web Study Guide
Andrew Roberts' web Study Guide
 Top
of
Page
Top
of
Page
 Take a Break - Read a Poem
Take a Break - Read a Poem
 Click coloured words to go where you
want
Click coloured words to go where you
want
To contact him, please
use the Communication
Form